Psoriasis - from the Greek word “psora” = “itch,” meaning “itching condition.”
Psoriasis can develop at any age, from infancy to adulthood, and approximately one-third of the cases can develop before the age of 2. Psoriasis varies from person to person, both in severity and how it responds to treatment. There are many rashes in children and adolescents, and they may look a lot like psoriasis; so, it’s important to get your child the correct diagnosis.
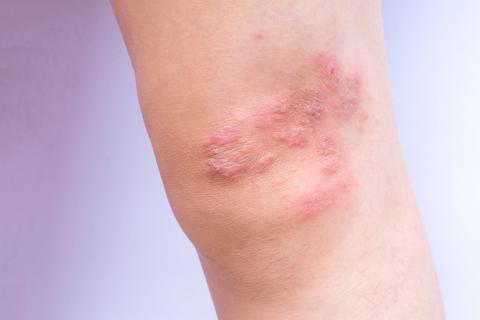
Psoriasis usually appears as dry, red, scaly patches and plaques on the skin. It can be very itchy at times, as the name suggests and even painful. Psoriasis can come and go in an unpredictable way which gives the characteristic of a chronic disease.
We don’t know what causes psoriasis, but we do know the immune system and genetics play a significant role in its development. In patients with psoriasis, the immune system is activated by mistake, resulting in a faster growth cycle of skin cells, and instead of falling off, the cells pile up and form thick, red, scaly plaques. Psoriasis tends to run in families. If one parent has the condition, there is a 25% chance that each child will have it.
Psoriasis can affect different parts of the body. It can be only on the skin (most common over elbows, knees, and scalp), nails (small depressions, ridges, yellowing, or thickening), and in some cases, the joints (called psoriatic arthritis). The most common type is called “plaque psoriasis,” which can be limited to a few plaques or involve large skin areas. The second most common type is “guttate psoriasis” which, instead of larger lesions, causes small red spots that mimic the pattern of drops of water. These spots usually appear on the arms, legs, and torso. Particularly in children, psoriasis may present on the face, scalp, behind and in the ears and groin, on initial presentation.
Types of treatments
It’s important to emphasize to affected children and teens that psoriasis is not contagious. Bacterial infections like strep throat may trigger psoriasis for the first time in children. Also, certain medications and medical conditions may be more likely to trigger psoriasis in a susceptible child or young adult.
Treatment of psoriasis depends on the type and severity of psoriasis and the area of the skin that is affected. The goal is to reduce the inflammation of the skin (which means decreased scaling, redness, itching, or discomfort of the skin).
At the Division of Dermatology at Phoenix Children’s, we offer the latest treatments and will develop a comprehensive treatment plan for your child or teen. Topical medicines may be prescribed and are applied directly to the psoriasis rash. These may contain topical corticosteroids or other non-steroid anti-inflammatory medicines. Vitamin D creams, coal tar solutions, salicylic acid, medicated moisturizers and shampoos, and topical retinoids are other therapies that may be added to your child’s treatment plan. These topical medications are often prescribed in combination with each other.
When topical medications are not as effective and the disease is widespread, some of our patients will benefit from ultraviolet (UV) phototherapy, which we currently offer at Phoenix Children’s. Phototherapy uses a narrow-band of UV-B light to reduce the inflammation of the skin. The excimer laser, also a targeted form of UV-B light, is an alternative that offers similar benefits. Those treatments are given 2-3 times per week in the clinic by specially trained providers.
In severe cases of psoriasis (which may also be associated with joint disease), and in cases where rapid improvement is needed, we use systemic medications. These are taken orally and include methotrexate, acitretin and cyclosporin. Other medications can be given by injection. They are called “biologics.” These are medications which target specific inflammatory mediators that cause psoriasis and its symptoms. There are many biologic medications approved for young children and teens currently with excellent safety profiles and minimal monitoring required allowing many patients to have clear skin.
It’s important for older children, teens and their caregivers to know that even pediatric patients with psoriasis are at risk for suffering from obesity, diabetes (high blood sugar), high cholesterol and heart disease later in life. The key is to maintain a healthy weight by eating a well-balanced diet and staying physically active. The whole family should be part of this healthy lifestyle.
Phoenix Children’s Division of Dermatology also participates in the latest clinical trials for pediatric patients with psoriasis, click here for more information.
