
Kayla may technically only have half a heart, but in spirit, she has enough heart to fill an entire room. These days, she’s full of laughter and smiles, despite having had two open-heart surgeries before her first birthday.
“You wouldn’t be able to tell the difference if we never said a thing,” said her mom, Karen. “She truly is our miracle child.”
Kayla and her parents, Karen and Matt, have been through a lot to get to this point.
The anatomy scan that changed everything
Karen and Matt had been wanting kids for a while. When Karen finally got pregnant, they were on cloud nine. They believed everything was fine, until Karen had an anatomy scan at 19 weeks.
Karen could tell something was wrong. The scan took an extra-long time, and her doctors kept looking closer at the baby’s heart area, taking different pictures. They were studying the scans closely. Finally, a high-risk doctor met with them, expressing concerns about the baby’s heart.
“We can’t really see a lot of the left side,” Karen recalled him saying. The doctor said there were many different things it could be, one being something called hypoplastic left heart syndrome (HLHS). To learn more, the doctor needed Karen to go to Phoenix Children’s for an echocardiogram, which is an ultrasound of the heart.
Kayla’s HLHS diagnosis
When Karen and Matt got home after the anatomy scan, they researched everything about HLHS online and worried about worst-case scenarios. However, in the back of their minds, they hoped everything was fine.
At Phoenix Children’s, they met Robert Puntel, MD, medical director of inpatient cardiology. He performed an echocardiogram, or echo for short, to get a better look at Kayla’s forming heart.
“Dr. Puntel was the nicest person in the world,” Karen shared. “I’ve never had a doctor spend so much time with me. He stayed with us through the whole echo, which takes about an hour, and explained what he saw.”
After the echo, their fears were confirmed: Kayla had HLHS, which is a type of heart defect, present at birth, that impacts how blood flows through the heart. During pregnancy, the left side of the baby’s heart doesn’t form properly, and when the baby is born, the heart can’t pump enough oxygen to the rest of the body. Babies with HLHS need multiple high-risk surgeries to have a chance of surviving.
Karen and Matt asked a lot of questions and, after weighing their options, decided to move forward with the heart surgeries for Kayla.
“I gave myself a couple of weeks to grieve the idea of not bringing home a typical heart healthy-baby from the hospital,” recalled Karen, “because Kayla would be in the cardiovascular intensive care unit for a month or more. But after that, I was ready to move forward – positive and focused on staying calm, doing what’s best for her.”
From birth, right to open-heart surgery
Karen knew that she wouldn’t have much time with Kayla immediately after she was born, but getting skin-to-skin time with her daughter was important. After confirming it was safe, she held her baby girl for 15 minutes. It was a huge win.
Because Kayla needed to be intubated a few hours after she was born, she went directly to the Cardiovascular Intensive Care Unit (CVICU) at Phoenix Children’s. There, although her oxygen levels were good in her lungs, oxygen wasn’t getting to the rest of her body – resulting in Kayla having her first open-heart surgery at only 3 days old. Typically, babies with HLHS have this procedure in the first few weeks of life.
The first HLHS surgery is called the Norwood procedure. It helps the right side of the heart also do the work of the left side since, with HLHS, the left side is either missing or very small. After the surgeon adjusts the right side of the heart, it pumps blood to the lungs and the rest of the body. Kayla’s first surgery was a success.


Caring for Kayla at home
Kayla stayed at the hospital to recover from her first surgery for about a month until her parents were able to take her home. Karen remembers long nights at the hospital.
“It was hard leaving her there because it goes against every natural instinct as a mother to go home without your brand-new baby every night,” she shared.
When Kayla finally was able to come home, her parents were relieved but also scared. The time period between surgery one and surgery two is called the interstage. For Kayla, the second surgery would happen at 4.5 months of age.
Karen and Matt had to learn completely new skills beyond what is required of most first-time parents. They checked Kayla’s oxygen levels with the pulse oximeter she wore 24/7. They had to weigh her frequently and keep her comfortable because excessive crying could disturb the shunt in her heart. Kayla had a nasogastric (NG) tube, so they could feed her with a pump, as well as lots of medications.
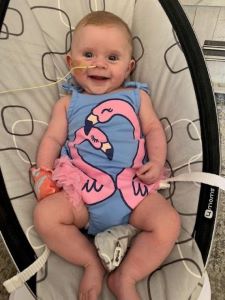
It was a lot for Karen and Matt, but they felt supported by their interstage team, led by Joseph N. Graziano, MD, medical director of the Single Ventricle Interstage Program and director of the Cardiac Catheterization Program and coordinator Susan Park, CPNP, MSN, CCTC.
“They are there for you any time,” Karen said. “You can message the interstage team if you have questions. They make themselves available to you because they know it’s a very unstable period. There’s also a therapist to talk through the interstage and prepare for the second surgery.”
Heart surgery No. 2 – the Glenn shunt
At 4.5 months old, Kayla received her second heart surgery called the Glenn shunt procedure. This surgery helps reduce the strain on the right side of the heart. It allows oxygen-poor blood from the body to go straight to the lungs instead of passing through the heart first.
After the second surgery, which was easier than the first, Kayla stayed in the hospital for a little over a week before going home to make a full recovery.
Making the most of each day
Before Kayla was born, Karen was a planner. She always worried about the next day. Now, she enjoys every moment. The entire HLHS process has taught her a lot, and she hopes her experience can help other parents in similar situations.
“It’s important to take some time,” Karen shared. “Then, move forward, and be present. It’s scary, but pay attention to what’s happening, so you can ask questions and advocate for yourself and your child. I wrote lots of notes in the hospital. Also, use all the resources at Phoenix Children’s, even if you don’t think you need them. At least do a consult. We assumed we didn’t need palliative care thinking it was hospice, but they were so wonderful while we were in the hospital. They would meet with us, re-explain things and let us ask more questions. They stayed after the doctor had left to make sure everything made sense.”
Today, Kayla is doing well, learning and exploring the world like a typical 1-year-old. She recently celebrated her first birthday with an Elmo-themed celebration. Without her NG tube, she really enjoys food. Her favorite is by far mac and cheese. Karen and Matt love watching her personality shine.

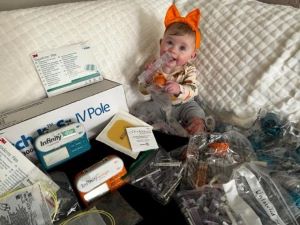
In the future, there are plans for Kayla to have one final surgery, called the Fontan procedure, when she’s between 3 and 5 years old. For now, though, Karen hopes that Kayla experiences every day to the fullest.
“We’re not going to limit her,” she said, “but we’re going to teach her that she has a special heart. And sometimes it’s okay to take a break if she needs to. She’s the strongest person we know, and she amazes me every single day. Even after everything we’ve been through, we’d do it all over again to have her in our life.”
